When the doctor is out
Training community medical officers to do acute surgery is saving lives in the small west African country of Sierra Leone.
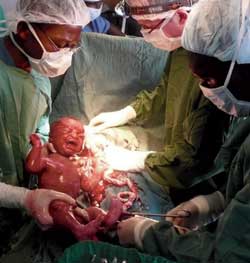
Community medical officers trained by CapaCare will be able to take care of acute surgical needs such as emergency births by Caesarean section.
Photo: CapaCare.org
In most parts of the world, a baby on the way means good news. In the small West African country of Sierra Leone, it can mean death. But a Norwegian surgeon and PhD candidate’s project to train health care officers to offer life saving surgery could help change all that.
Sierra Leone was ravaged by civil war from 1991 to 2002, which destroyed much of its governmental infrastructure, crippling its ability to offer basic health care services. Ten years on, the government is still rebuilding its health system, its efforts hampered by the fact that there are only 10 surgeons and roughly 120 doctors in the entire country.
Scientific documentation
Håkon Bolkan, a surgeon and PhD candidate in NTNU’s Faculty of Medicine, believes that 80-90 per cent of the acute surgical needs in Sierra Leone can be successfully treated by specially trained health care workers. And in 2011, he started a non-profit organization called CapaCare to offer health care workers training in acute surgical procedures.
But the Sierra Leone government needs solid proof this different approach to surgery can work, Bolkan says. His PhD research will provide the scientific documentation, and in doing so, could help change the face of the health care delivery system in one of the poorest African countries.
“The (government’s) initial reaction to training community medical officers is ‘So you are offering us substandard care?’” he says. “Or they say, ‘You would never do this in your own country.’ One of the reasons I’m doing this PhD is that we need hard results for advocacy.”
Civil war, no infrastructure
Just a few years ago, the maternal death rate in Sierra Leone was among the highest in the world – a fact that led government officials to start a programme to offer free care to pregnant women and nursing mothers.
While mortality numbers have started to drop, they remain problematic. In 2008, 1037 Sierra Leonean mothers died for every 100,000 live births – or just over 1 per cent. That’s a risk that’s 135 times greater than in Norway. “To become a mother is not a happy thing in Sierra Leone,” Bolkan says.
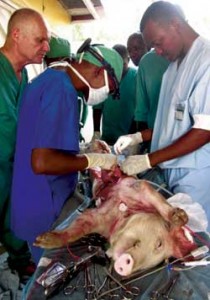
The CapaCare students first practice their surgical skills on pigs, where they learn everything from administering anaesthesia to suturing intestines.
Photo: CapaCare.org
Maternal mortality is only one of Sierra Leone’s many health care challenges. The country ranks 180 out of 187 nations on the UN’s Development Index. In fact, one 2010 study found that surgical conditions in Sierra Leone were far worse than those in the United States during the US Civil War of 1861–1865.
For example, while 10 Sierra Leonean government hospitals provide surgical care for 80 per cent of the country’s population, each hospital averaged just 135 beds, which limited the number of surgeries each could offer to just over 300 per institution. In contrast, the US Union Army in 1865 had access to 206 hospitals with nearly 140 000 beds, the study found.
And while an average European or American citizen might have 9 surgeries over the course of his or her lifetime, the surgical capacity in Sierra Leone is so low that only 1.5 surgeries are performed per 1000 people, on average, Bolkan says.
Changing the surgical picture
Bolkan and his colleagues at CapaCare know they can’t change the infrastructure deficiencies in Sierra Leone overnight. But “it’s surprising what you can do with no running water,” Bolkan observed. “We can do so many things.”
With the CapaCare training, 29 community medical officers or other health care providers will learn how to do basic surgical procedures, such as hernia repairs, Caesarean sections, appendectomies and setting compound fractures.
The organization started its training in January 2011 with two community medical officers, and adds two more to the training rotation every three months. Each trainee has 2 full years of instruction and practice, with training in district hospitals throughout Sierra Leone. The Kavli Fund, the Lion’s Club and St Olavs Hospital in Trondheim are supporting the effort. The hospital has also adopted the programme and is supplying personnel for training as part of its international outreach efforts.
Saving lives
Emmanuel L. Tommy was one of the first community medical officers to sign up. Since his training began, Tommy, soft spoken and calm, has been involved with more than 400 operations, roughly half on his own. He, too, has first-hand experience with Sierra Leone’s limited medical system. He lost his mother when she was just 48, and two of his eight siblings also died young.
Emmanuel says that before his training, he watched his patients die because he didn’t have the expertise to help them. A poor road network and long distances to surgeons and hospitals makes transferring patients impossible, even though they might only need simple surgery. “I have seen a lot of people dying in these communities that I could not help, because I did not have the surgical skills,” he said.
At a glance
What: CapaCare, a medical humanitarian organization designed to provide medical education and training to increase the level of skilled staff at district hospitals in Sierra Leone.
People: Håkon Bolkan, a surgeon and PhD candidate at NTNU is chairman of the board,. He started the organization with Brynjulf Ystgaard, a surgeon from St Olavs Hospital. Many volunteers come from across the globe, including from St Olavs Hospital in Trondheim, which has adopted the project as part of its international outreach efforts.
Goal: To train 29 community health officers and young medical doctors in Sierra Leone to undertake life-saving surgeries by the end of 2016.
Support: the Kavli Trust, the Lions Club, St Olavs Hospital in Trondheim, Friends of Masanga in Denmark.
Website: www.capacare.org
That’s all changed, as Emmanuel enters his last phase of training. Not long ago, he says, a woman about to give birth came to him in pain – and it turned out that her uterus was turned upside down, with the baby trapped inside. Without access to a Caesarean section, the woman and her baby would have died. But Emmanuel was able to undertake the life-saving surgery and mother and child are doing well.
How it works
The training starts at Masanga Hospital in Tonkolili, a former leprosy hospital that was destroyed during the Civil War, but that has been rehabilitated by a Danish non-profit group called Friends of Masanga. There, students are given between six and nine months of formal training in everything from sterile procedures to diagnostics and surgical techniques.
Early on, trainees practice their different skills on pigs, including giving anaesthesia, inserting chest drains, removing a damaged spleen, packing a bleeding liver, and sewing intestines. From there, students graduate to assisting with operations, and then in the end, to doing operations on their own. Roughly 30 surgeons, nurses and anaesthesiologists, many drawn from St Olavs Hospital in Trondheim, have helped with the programme.
After their first rotation at Masanga, the trainees are sent to two or three other district hospitals. The training requires each participant to contribute not only with their time, but also by leaving their families to work in the different parts of the country.
And while each trainee continues to be paid during the course of the programme, the actual amount is roughly half of what they would make in their work as a community health officer. Tommy, for one, says he’s willing to make these contributions because he wants to help make fundamental changes to Sierra Leone’s health care system. “I want to be a part of the people who write history in this country,” he says. “I want to help my people.”
A little piece in a larger puzzle
Sigrun Aase Holen, a surgical nurse from St Olavs, travelled to Masanga Hospital in late 2011 to help teach sterile technique to the trainees – a challenging assignment given the lack of a steady electricity supply, the only source of which was an ageing and overworked generator.
“In the end we managed without electricity, and thanks to some headlamps we brought with us, we were able to do a hernia operation and run the surgical ward,” she wrote in a blog entry about the experience.
Holen subsequently joined CapaCare as a board member. She says that she feels that she benefitted as much from experience of helping people in Sierra Leone as the people whom she trained. “I was very glad to be able to participate as a little piece in the larger puzzle of how we handle health care challenges,” she said.
Measuring success
But all the training in the world won’t matter if in the end, the Sierra Leonean Ministry of Health and Sanitation doesn’t certify the trainees or build them into the country’s health care services.
Although a similar approach to surgical care has been adopted in Mozambique and in southeast Asia with good results, Bolkan’s PhD is a critical piece of demonstrating that these kinds of programmes can work.
Bolkan’s work starts with documenting the current surgical situation in Sierra Leone, before the CapaCare trainees are officially employed in the health care system. Once the trainees graduate, they will keep careful records of number of surgeries and patient outcomes, with which Bolkan will be able to document the impact they have, along with other parameters, such as the cost of training “I believe that if this programme goes on for some years, (the graduates) will become the backbone of surgical care in the district hospitals in Sierra Leone,” Bolkan says.