Doctor duo designs emergency room triage
Proper and prompt treatment in the emergency room saves lives. With help from Norwegian doctors, a hospital in Nepal has started to sort patients into red, yellow and green categories. The system has made a difference.
Imagine an emergency centre in Nepal where sick and injured patients are waiting for medical attention. The waiting room is full, and people are queued up outside. Then a woman enters who has just given birth. She is bleeding heavily and is weak from losing blood. Soon after, five young men and three elderly women arrive. They all have major fractures and lacerations after a serious traffic accident.
Many of them travelled a long way to get here. Some came by bus, some on foot, and some by horse or ox. Few arrive by ambulance.
The queuing system in the emergency room is set up on a first-come, first-served basis. The doctors and nurses barely consider the extent of the patient’s injury, In the worst cases, people die while waiting to be examined and get help.
This is the situation in hospitals in Nepal and in many other poor countries. However, a research project led by NTNU and St. Olavs Hospital in Trondheim is working to improve the situation considerably.
“We saw that we had a lot to gain by introducing the same emergency room procedures in Nepal that we’ve established in Norway,” says Dr. Erik Solligård.
Vision 2030
- The Norwegian Ministry of Foreign Affairs, Ministry of Health and Care Services and Ministry of Education and Research have asked for input from Norway's major educational institutions on how to improve the nation’s global heath and education initiatives through the Vision 2030 initiative.
- NTNU is among the institutions that have submitted a response.
The project is part of “Vision 2030” (see fact box).
- You might also like: Ebola’s deadly toll
Long-term cooperation between NTNU and Nepal
NTNU has worked with Kathmandu University for many years. This partnership is primarily built around research and education related to hydropower. But connections with Kathmandu University have also gradually grown in other disciplines, and in 2009 NTNU’s Faculty of Medicine expanded the collaboration.
The Faculty announced the availability of project funding, and this is where the doctor couple and researchers Kari Risnes and Erik Solligård came into the picture. Risnes is a paediatrician and Solligård is an anaesthesiologist. Both are associated with NTNU and St. Olav’s Hospital. Through cooperation with Kathmandu University they saw an opportunity to help spread knowledge and share experiences.
New training programme
“We have established good emergency room care procedures in Norway. We work in teams and everyone knows their roles. It’s important to identify what the sick or injured patient needs immediately upon arrival so that the patient receives proper treatment as quickly as possible,” says Solligård.
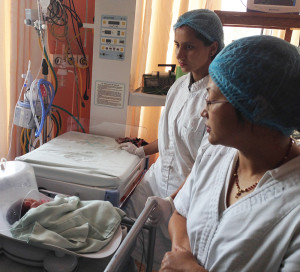
Newborns and their mothers are a vulnerable group when it comes to disease and mortality. (Photo: Erik Solligård)
In the first phase of the project Risnes and Solligård established collaboration between the Medical Simulation Centre at St. Olavs Hospital and NTNU. Using equipment and expertise from the simulation centre, Risnes and Solligård created a training program for medical and healthcare professionals at Dhulikhel Hospital, which cooperates with Kathmandu University.
“We concentrated initially on birth complications and acute infections. We created a training scenario and put together teams who were trained for emergency situations and effective coordination,” says Risnes.
Risnes and Solligård brought along training dummies that could “breathe” and “talk,” so that they could measure pulse and heart rate and create as realistic a situation as possible. The training scenarios were videotaped, enabling the team to review the situation afterwards and evaluate themselves.
Through their teaching and guidance, Risnes and Solligård built up expertise in the hospital so that local health professionals could eventually run their own training.
Increased standard of living and a lot of traffic bring new patients
The second phase of the project was to track the course of patients’ illnesses. The hospital had little overview in this area, reflecting the fact that the influx of patients has increased and that they have different injuries and diseases than before.

The traffic situation has changed a lot in a short time, and a large increase in the number of road accidents is increasing the patient pressure on hospitals. (Photo: Erik Solligård)
According to Risnes, traffic on the roads has increased tremendously in recent years and the disease picture is partly characterized by large, serious bus and moped accidents. WHO defines the increase in traffic accidents in some Asian countries as an epidemic, she says.
“We also have a new group of patients, those with lifestyle diseases. As the standard of living has increased in Nepal, the proportion of people with diabetes and cardiovascular disease has likewise grown. And for cardiac patients early treatment is very important,” says Solligård.
People who are injured in mudslides constitute another group that poses a challenge for emergency centres. Periodically, large landslides and mudslides cause serious injury to high numbers of people.
Dhulikhel Hospital maintains a good standard, given the conditions. Yet because there is very little in the way of patient records, many patients end up in the emergency room for their discharge diagnoses and treatment outcomes.
- You might also like: When the doctor is out
The sickest treated first
The survey that Risnes and Solligård initiated can now provide an overview of the various patient groups and disease patterns. This knowledge is helping more people get proper treatment and ensuring that those who need it most receive treatment first.
“We have helped to describe what ails patients and to define degrees of severity. This helps health personnel at Dhulikhel Hospital prioritize and sort patients to determine who is sickest, who should be treated first and how they should be treated,” says Solligård.
This sorting system of patients is called triage. It is like a traffic light system where patients are placed in categories of red, yellow and green.
“We’ve mapped out the disease picture of those who come to the emergency room. Now we have a systematized knowledge about what kind of injuries or diseases patients come with, as well as the scope of the various categories. Handling of patients used to be based on what health care providers thought the situation was. Now it’s based on facts,” says Solligård.
Creating a new patient registry
This survey work has led to the development of a database of 8,000 patients, which four Nepalese research assistants have been involved with. They have contacted patients one month after discharge to chart their medical history.
Risnes points out that in this part of the world only a limited overview of disease prevalence exists. And, she says, we need to remember that it has only been 30 years since Norway started to conduct its own Nord-Trøndelag Health Study (The HUNT Study), a longitudinal survey that has provided an enormous amount of knowledge about the health of the Norwegian population.
Phase Two of the Nepali project consisted of:
- Introduction of systematic patient prioritization by degree of urgency.
- Structural adjustments to allow for separation of patients into various categories, including distinguishing infectious conditions from non-infectious ones.
- Defining urgency processes that lead directly to treatment, such as for births and acute bleeding.
- Creating response teams that quickly come to the aid of patients needing immediate treatment.
- Creating a disaster plan in the case of a mass influx of injuries or infections.
Building local expertise
Kathmandu University is responsible for the education of a large percentage of Nepalese doctors and nurses. Training a group of employees at the hospital in using simulation provides several benefits. These local employees are now adopting their new knowledge and the teaching principles they have learned to train their own health care personnel.
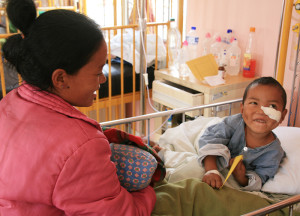
A little boy is on the mend after receiving prompt, good treatment at Dhulikhel Hospital. (Photo: Erik Solligård)
The goal has always been to build expertise locally, and the Nepalese research assistants have been important partners. In addition, nine medical students from NTNU have done fieldwork for their master’s theses on this project, and now a Nepali PhD candidate has started on a doctorate at NTNU.
“It’s important to have institutional cooperation between NTNU and Kathmandu University. When cooperation is close, then projects have an overarching structure and an anchor that ensure continuity,” the couple says.
“Another strength of this project is that doctors stay at- or return to- Dhulikhel Hospital. Brain drain is minimal, partly because doctors go abroad periodically. This both builds and maintains competence.
Measuring effects
The project in 2015 is now entering its third phase, where the effects of the changes are being analyzed and measured.
The expected effects of Phase Three are:
- Reduced mortality.
- Better resource utilization, so that the most acute and critical cases get priority access to the best expertise.
- Better utilization of bed capacity, because more competent decision-making by staff enables patient assessment to occur early in the treatment sequence.
- Reduced time to treatment for acute life-threatening disorders.
- Improved local expertise in planning for a mass influx of patients.
- Improved expertise and readiness for infectious epidemics.
- Development of expertise in change management and research in the institution where the project is executed.
- Patient registry that provides access to management data for the institution’s own operations.
- Knowledge about disease prevalence, which can contribute to the planning of necessary strategies for fighting disease.




