Good cholesterol is getting even better
Cholesterol is far better than its bad reputation. Good HDL cholesterol can actually limit atherosclerosis.
CHOLESTEROL: HDL cholesterol can reduce the inflammation that leads to arterial plaque build-up.
Atherosclerosis, or hardening of the arteries, develops when plaque— particularly cholesterol, fatty substances, cellular debris and calcium deposits—accumulates on artery walls. It is widely accepted that atherosclerosis develops as a chronic inflammatory process.
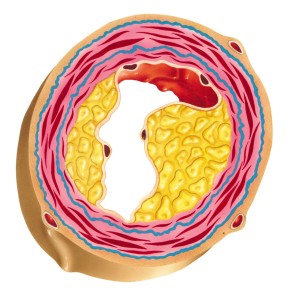
Atherosclerosis is due to the accumulation of fatty substances in the vessel wall, particularly cholesterol, inflamed cells and deposits. Illustration: Thinkstock
Understanding the mechanisms that affect the immune system in this process is fundamental to developing better treatment for patients with atherosclerosis.
“We’ve shown that “good cholesterol,” which consists of high-density lipoproteins, dampens the chronic inflammatory reaction that leads to atherosclerosis. HDL cholesterol also has several other positive characteristics,” says Nathalie Niyonzima.
Niyonzima is a researcher at CEMIR, the Centre of Molecular Inflammation Research at NTNU.
“We’ve been looking for mechanisms that trigger and influence an inflammatory response. The hope is to move from lab studies to clinical trials,” says her colleague Eivind Samstad. Their findings were published in The Journal of Immunology this summer.
Cholesterol Crystals
Cholesterol that accumulates in the blood vessel walls results in the precipitation of cholesterol crystals, previously thought to be inert.
However, a few years ago researchers at CEMIR discovered that these cholesterol crystals actually play an essential role in triggering the immune response that leads to the development of atherosclerosis.
As Niyonzima explains, the immune system identifies the cholesterol crystals as harmful substances in the body that need to be removed. But the antibodies that come to the body’s defence are unable to break down the crystals. The immune system calls out for reinforcements, and more antibodies arrive, to no avail. The immune reaction runs wild, and the inflammation process escalates.
Local blood samples
To test the effect of cholesterol crystals, researchers used blood samples from healthy volunteer donors – many of whom were colleagues in the same department.
“I needed to thank a lot of people for their contributions when I defended my dissertation this spring,” Niyonzima said with a smile.
“In healthy blood samples all the natural components are present, allowing us to study all the mechanisms. When we added cholesterol crystals, we saw that the complement system—an important part of the innate immune system—was activated,” she said.
Adding the cholesterol crystals triggered an immune reaction that eventually got out of control, resulting in inflammation.
“Researchers at CEMIR were the first to show that cholesterol crystals can trigger inflammation by activating the complement system. Now other studies have confirmed this result,” says Niyonzima.
Good cholesterol
Now the researchers have gone further and looked at the effect of HDL, also called “good cholesterol.” It counteracts the effects of “bad cholesterol,” or low-density lipoproteins (LDL).
Traditionally, HDL has been perceived as beneficial because it carries away cholesterol from the artery walls. It also has several other good qualities: among other things, it is an antioxidant, and it protects blood vessels’ surface cells. So it turns out that the good cholesterol, or at least an artificial variant of it, helps to slow the inflammatory process caused by cholesterol crystals.
CEMIR researchers used reconstituted HDL, developed by the Australian pharmaceutical company CSL Behring, where one protein fraction is cultivated.
“Our study shows that reconstituted HDL, or rHDL, binds cholesterol crystals so that they don’t trigger the complement system. This action dampens the inflammatory response and reduces the risk of atherosclerosis,” says Niyonzima.
She adds that these findings suggest that it may be necessary to supplement existing treatment regimens for atherosclerosis.
Examining inflammation
Samstad took his doctorate at CEMIR and is now a doctor at the hospital in Ålesund.
“Over the last decade, scientists have been concentrating more on the inflammation associated with atherosclerosis. But there’s still a lot of debate about what triggers this inflammatory response,” says Samstad.

By reducing the amount of saturated fats and transfats you consume, you can decrease your risk of atherosclerosis. Photo:Thinkstock
Drugs that reduce LDL cholesterol levels in the blood have been the main treatment for atherosclerosis. Samstad believes that we’re now seeing a shift toward a greater interest in anti-inflammatory medications.
“When we go in and influence an important mechanism like the immune system, it’s critical that we know what we’re doing. We need to know what mechanisms we’re affecting, and how,” he says.
So far, researchers have used blood from healthy donors. Samstad hopes they have the opportunity to follow up their study with an actual patient group, such as people who have had heart attacks.
Follow-up projects
CEMIR has been designated a Centre of Excellence (SFF) for research. A key question for the centre is how inflammation may be so closely associated with many seemingly different chronic diseases.
“We have a number of different projects that focus on studying the inflammatory mechanisms and trying to find ways to inhibit inflammation,” says the centre’s director, Professor Terje Espevik.
The many exciting discoveries point towards larger clinical trials. But studies such as these are too expensive for a research centre like CEMIR.
“Our role is rather to conduct what is called translational research, providing basic discoveries that serve as the basis for clinical trials. The pharmaceutical industry can take the ball from here,” Espevik says.
In the wake of their rHDL project work, CEMIR scientists are also working with another substance, which appears to have at least three important characteristics: it dissolves cholesterol crystals, it is powerfully anti-inflammatory, and it transports cholesterol back to the liver.
“I think we’ll be coming with more exciting news before too long,” says Espevik.
Reference:
“Reconstituted High-Density Lipoprotein Cholesterol Attenuates Cholesterol Crystal-Induced Inflammatory Responses by Reducing Complement Activation.” The Journal of Immunology, June 2015.