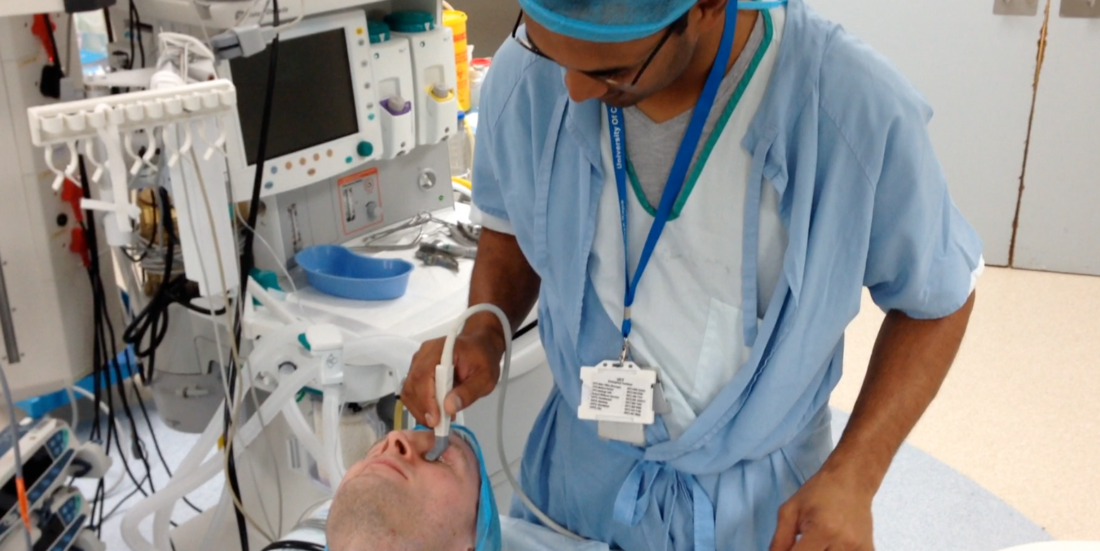
Ultrasound detects high cranial pressure
An anatomical discovery, combined with Norwegian ultrasound technology, is about to save lives and prevent brain damage.
Norwegian ultrasound researchers have for some time been collaborating with one of Africa’s largest children’s hospitals – the Red Cross War Memorial Children’s Hospital in Cape Town. The aim of this joint effort is to transfer and share knowledge about using ultrasound as a 3D navigation system for surgeons, with the result that a new diagnostic tool has been developed that can detect raised intracranial pressure (ICP).
High levels of head injury in South Africa
Llewellyn Padayachy is a pediatric neurosurgeon at the hospital. An important part of his job is to treat children suffering from head injuries, including those resulting from the many traffic accidents that occur in South Africa.
Having worked with Norwegian researchers who use ultrasound both as a diagnostic tool and a navigation device during surgery, Padayachy came up with an idea – to apply ultrasound to image and map pressure in the brain.
Increases in ICP can result in damage to both the brain and spinal cord. Currently, these kinds of increases are detected directly using a sensor that is surgically inserted into the patient’s head. This procedure must be carried out in an operating theatre. It is expensive, demanding and, not least, stressful for the patient.
Minute physical changes
Padayachy’s theory was that the optic nerve sheath extending from the eyeball into the cranium would be affected by pressure fluctuations in the patient’s head. He believed that there would be variations not only in the diameter of the optic nerve sheath, but that its dynamic properties would also be affected. His hope was that these changes could be detected using ultrasound images taken from a patient’s eyelids, perhaps providing real-time data that could help save lives.
In order to detect these minute changes in the nerve sheath it was necessary to devise new analytical methods. After the research team had analysed ultrasound images from patients that had previously been treated at the hospital, they discovered a small but significant difference in the optic nerve sheath. The sheath is soft under normal ICP conditions, but stiffens in response to increases in pressure exerted by the spinal fluid. In collaboration with Padayachy, the researchers then started to develop an entirely new ultrasound-based tool capable of detecting the microscopic changes in the nerve sheath tissue.
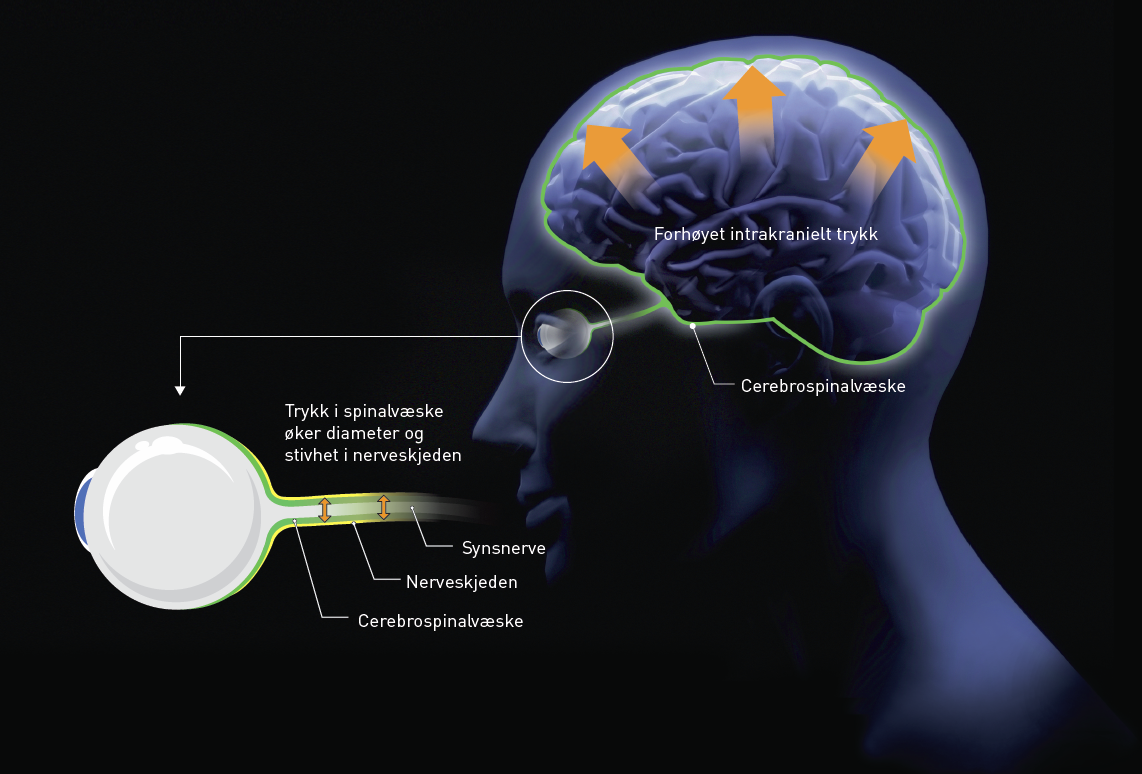
Increased intra-cranial pressure (ICP) can lead to damage to both the brain and spinal cord. Currently, ICT is detected using a sensor surgically inserted into the patient’s cranium. A new method can achieve the same result simply by scanning the eye with an ultrasound probe. Illustration: Doghouse/Knut Gangåssæter.
From brain tissue to the nervous system
SINTEF researchers Reidar Brekken and Tormod Selbekk have in fact been working extensively on approaches to ultrasound signal processing as a means of detecting small brain tissue deformations, and their efforts are now bearing fruits.
“After three years of work supported by in-house funding, we have transformed an idea into a real diagnostic tool”, says software developer and Senior Research Scientist Reidar Brekken. He goes on to explain;
“The tool comprises an in-house developed algorithm that analyses ultrasound images of a patient’s optic nerve sheath in order to detect minute changes in its motion patterns. Using this tool will make it possible to measure ICP simply by means of a doctor scanning the patient’s eye with an ultrasound probe. And the diagnosis is immediate, for instance in an ambulance at the scene of an accident. The tool will make it possible to make an early diagnosis without the patient requiring surgery”, says Brekken.
This technological and clinical innovation has resulted in a recent article in the respected periodical Neurosurgery.
Patients will be contributing to future developments

The Norwegian scientists Tormod Selbekk (t.v.) og Reidar Brekken together with Llewellyn Padayachy at Red Cross War Memorial Children’s Hospital.
The researchers will now be trying the method out on a larger group of patients in order to verify the accuracy of their measurements.
“We’re planning a number of clinical studies, both at the Red Cross War Memorial Children’s Hospital and the Department of Neurosurgery at St. Olav’s Hospital in Trondheim”, says Tormod Selbekk. “Work is now underway to obtain funding for the development and verification of the concept so that an instrument can be developed for practical application in clinics”, he says.
Selbekk emphasises that it is vital that patients with high ICP receive treatment as soon as possible. Without the right treatment, high ICP can result in brain damage, disability and, in the worst case, death.
“An instrument that makes it easy to measure ICP can make a major contribution to quicker diagnosis and treatment”, he says. “The technology that has now been developed has great potential to promote a better life for a very large group of patients”, says Selbekk.