Super quick COVID test uses new technology
The ability of gold particles to reflect light in different colours is used in applications from stained glass to pregnancy tests. Now researchers are set to exploit the same properties in an ultra-fast sensor for the coronavirus.
Sticking swabs up our noses and down our throats to confirm or deny whether we are infected with the coronavirus – almost all of us have done it multiple times in the last couple of years.
The methods that have been used to detect and prevent the spread of the virus have been the same around the world, either:
- the expensive, time-consuming but very accurate PCR method where the DNA of the virus is detected in our mucous membranes, or
- the simpler and faster method that only indicates whether we have developed antibodies against the virus.
Ultra-fast detection
However, both methods have their weaknesses. The PCR method is expensive and time-consuming, while the antibody method does not tell us anything about whether we actually have the virus in the body. A simple and affordable way to detect the virus that provides a quick result would therefore be helpful.
Now researchers from NTNU, Oslomet and the University of Tabriz in East Azerbaijan have demonstrated a method for detecting coronavirus in blood samples using nanosensors.
“A lot of research focuses on finding methods to quickly isolate infected people, which can break the chain of infection. Nanosensors have received a lot of attention due to their unique properties for ultra-fast detection of particles such as viruses,” says Amir Maghoul. He is a researcher and the first author of the article “An Optical Modeling Framework for Coronavirus Detection Using Graphene-Based Nanosensor”. He was a post-doctoral fellow at NTNU when he started his work.
A first step on the pathway to developing a separate nanosensor for the coronavirus is to identify the optical properties that distinguish the coronavirus from other particles in our blood.
Ingve Simonsen, a physics professor at NTNU, explains.
Most people have seen the coronavirus depicted as a round core or ball with red “spikes” or stems sticking out.
“We wanted to see what role the length and size of these “spikes” play in how the cells reflect light, as well as whether the size of the nucleus matters,” says Simonsen.
- You might also like: New nanomaterial to replace mercury
Displaces resonance
To find answers to their questions, the researchers used mathematical models. The optical behaviour of the virus – that is, how the virus cell reflects light in the form of resonance – was simulated and analysed over the entire light spectrum.
“We observed that the reflectivity varied with the length of the spike proteins. As the spikes get longer, the reflectivity decreases at the same time as the resonance shifts to higher wavelengths,” says Simonsen.
The researchers observed the same response when they varied the size of the virus’ core in the models. The width of the spike protein had less effect on how the light was reflected. In this way, the researchers could find out in which part of the wavelength spectrum the coronavirus differs from other particles in the blood.
“At certain wavelengths, we get a different optical response depending on whether viruses are present or not. We call this the optical signature of the coronavirus,” says Simonsen.
“We know that the optical properties of particles change depending on their environment. They behave differently if they’re in water or in a vacuum, if several particles are next to each other or if the surface is covered with a thin layer of another substance.”
- You might also like: How children are affected by coronavirus, RS virus and rhinovirus
Pregnancy test example
The first person to describe in general terms how spherical particles reflect light waves was the German scientist Gustav Mie in 1908.
“It is well known that ordinary light consists of a spectrum of wavelengths. This is what we see when we look at a rainbow or when light passes through a glass prism. The light hits water molecules in the atmosphere or the prism and is reflected in the light’s various wavelengths, which we see as a spectrum of colours,” says Simonsen.
Mie showed how small spheres or nuclei react differently to light.
“For example, small metal particles have a very strong optical response. This characteristic is used in certain types of pregnancy tests that measure the optical response to small gold particles,” Simonsen says.
“The hormone you look for in the urine – which you only have if you’re pregnant – collects on the surface of the gold particles on the test stick and changes the resonance frequency of the particle. The result is a colour change to blue, which shows that you’re pregnant.”
Rose painting example
Another example of how small particles react to light can be seen in stained glass, such as the large rose window in Nidaros Cathedral. The strong red, blue and green colours are all the result of the optical response of the metal particles used in the glass. And it is this property that can be used to detect coronavirus in blood samples.
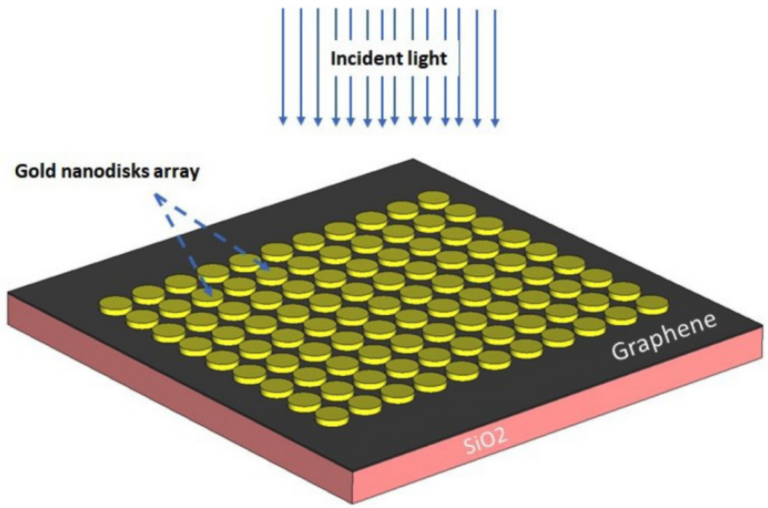
“What you do is place a network of thin, cylindrical gold particles over a very thin layer of graphene. Graphene is a nanomaterial with a lot of fascinating properties, including the fact that it conducts electricity well and with little loss.”
When blood containing the coronavirus passes over the gold particles, the resonant frequency of the particles changes, which in turn creates an electromagnetic field. This field sets up a current in the sensor that can be easily measured.
By studying the current curves for certain frequency ranges of the incoming light, we can determine whether the blood contains coronavirus or not,” says Simonsen.
Great potential for nanotechnology
Nanosensors have the potential to be very sensitive. The “smart” graphene material in the nanodisk acts as an amplifier, explains Amir Maghoul.
“Nanotechnology hasn’t been used before for this type of sensor, so this development is new technology. What we’ve done here is create the first optical framework to detect coronavirus and show how the virus behaves in the optical spectrum,” says Maghoul.
Now the next step is to establish a company that can develop a laboratory prototype for the nanosensor.
“We need to raise money so that we can go ahead and develop a sensor for common use. The collaboration between NTNU and Oslomet has shown that we have facilities with significant potential to develop and produce this type of nanosensor for biomedical use if the work is supported financially,” says Maghoul.
Watch a video that summarizes the article:
Reference:
Amir Maghoul, Ingve Simonsen et al.: An Optical Modeling Framework for Coronavirus Detection Using Graphene-Based Nanosensor. National Library of Medicine. DOI: 10.3390/nano12162868