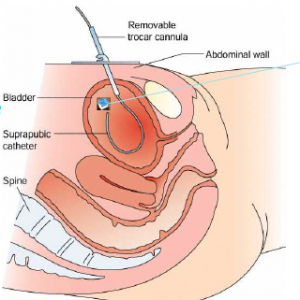
Lifesaving sensor for full bladders
A small pressure sensor can make the difference between life and death. The first tests on humans will be carried out in April on patients with spinal injuries at Sunnaas Hospital in Norway.
More than 220,000 people in Norway suffer from a neurological disease that means that they have difficulties with urinating and incontinence, and have problems controlling their bladders. About 3,000 of these are particularly badly affected. Spinal injuries can damage the nerve supply to the bladder, meaning that people cannot tell when their bladder is full and needs to be emptied. This then creates an excessively high pressure on the bladder, which affects the kidneys and can lead to damage that may be life-threatening.
FACTS:
• Measuring pressure is an extremely important medical practice. The need for new and improved measurements can be met using smaller, more reliable sensors.
• Routine measurements are for blood pressure and pressure in the brain, on the eye and in major joints.
• The aim of one of SINTEF's previous projects was to develop an integrated sensor in prosthetic hips.
Measuring pressure with a catheter
“Measuring pressure in the bladder is essential in order to see whether an operation is necessary, or whether the condition can be treated with medication. The measurements reveal how the bladder fills and empties”, explains Dr Thomas Glott of Sunnaas Hospital.
Currently, measurements are taken using a catheter which is inserted into the urethra so that the bladder can be filled with water. This is uncomfortable for the patient, and since the bladder is filled with saline at an unnaturally high speed, the method is also unreliable.
Pin sensor
For many years, researchers at SINTEF have been working on developing tiny sensors for measuring pressure in the body. When the chance to work closely with Sunnaas Hospital came up, they decided to focus on measuring pressure in the bladder.
Ingelin Clausen, who works in the MiNaLab at SINTEF ICT, demonstrates the tiny pressure sensor that looks like a pinprick on her finger. “Unlike a catheter, this sensor can be inserted under the skin”, she explains.
Thomas Glott adds that this is done by inserting a thin needle through the skin and into the bladder. “The sensor is positioned without causing discomfort to the patient, who can then move about normally without the disruptive catheter, and the risk of infection is reduced”.
Test plans
The sensor is now being tested on three patients. One long-term plan is to test the system on 20–30 patients.
“Working with Sunnaas has given us a great chance to try out our technology on patients. It has also provided a useful insight into other medical applications. Our long-term aim is to develop a method of implanting the sensor more permanently, since many patients need measurements to be taken regularly”, says Ingelin Clausen of SINTEF. “These would be sensors that could be implanted for several months or years”.
At the moment, the sensor is connected to a thin wire, but the next step would be to make it wireless. Another long-term option could be to allow the measurements to be read by a smart phone. That way, any increase in pressure could be detected even when patients are at home, thereby avoiding resource-intensive and uncomfortable examinations in hospital.