Norway’s Nobel laureates take up the fight against Alzheimer’s
Developing an effective treatment for Alzheimer’s disease is the long-term goal of a new national research centre in Norway. Nobel laureates Edvard Moser and May-Britt Moser will lead the K. G. Jebsen Centre for Alzheimer’s Disease, aimed at determining how Alzheimer’s disease arises in the brain and its early stages of development.
The Foundation Stiftelsen Kristian Gerhard Jebsen has donated NOK 22.5 million to a national centre for the fight against Alzheimer’s disease. Edvard Moser, from the Kavli Institute for Systems Neuroscience at the Norwegian University of Science and Technology, will lead the new centre, with May-Britt Moser as deputy head. The goal is to translate Nobel Prize-winning brain research from laboratory to patient.
Auguste D and Alzheimer’s diagnosis
The history of Alzheimer’s disease is long and painful. In 1901, a young German psychiatrist meets Mrs. Auguste Deter. Auguste was disoriented, suffering from memory impairment and hallucinations. She had lost much of her language and her husband was no longer able to care for her.

Auguste Deter’s family gave the psychiatrist Alois Alzheimer permission to autopsy Deter’s brain. This allowed Dr Alzheimer to give the world the first insights into how the disease that bears his name changes both the brain and the mind. Photo: Unknown.
“I’ve lost myself, so to say,” Auguste D. told her psychiatrist. What particularly amazed him was that the woman was in the middle of her life, barely 51 years old and far too young for the disability to be age-related.
Within five years, Auguste was dead. The psychiatrist wondered if her brain held clues that could shed light on the mental illness. With the family’s permission, he examined Auguste’s brain.
Never before had the psychiatrist held in his hands a human brain so severely atrophied. The shrinkage was particularly evident in the cerebral cortex, the outermost layers of the brain where the little grey cells that are so important for higher brain functions reside.
- You may also like: How your brain experiences time
The disease that changes the brain and the mind
To continue his search for signs of the disease, the psychiatrist had to look into the brain. Carefully, he cut the brain into thin slices, which he then coloured with silver salts to increase contrast. Under the microscope he found further traces of disease. Two different forms of accumulation had formed in the cortex of the brain tissue. One type was found in between brain cells, and the other had accumulated inside the brain cells.
Estimated numbers of the world's population affected by Alzheimer's disease
2018: 50 million
2030: 82 million
2050: 152 million
(Source: World Health Organization, 2018)
Today, these two accumulations are known as beta-amyloid plaques and neurofibrillary tangles of tau protein.
The young psychiatrist was Alois Alzheimer, and the illness he had discovered in Auguste Deter was named after him. Thanks to the Deter family, who gave their consent for Auguste’s brain to be studied, Alzheimer was able to give the world a first glimpse into how this disease alters both the brain and the mind.
Know where the disease starts
Today, more than a hundred years later, Alzheimer’s disease has become one of the greatest threats to public health. The world still knows little about what Alzheimer’s is or what causes the disease, and nothing is known about how it can be stopped. There is no effective treatment.
But researchers know where it all starts, deep inside the brain, in an area the size of a fingernail, called the entorhinal cortex. The area is closely interwoven with the brain’s memory centre, which suggested early on that this area had an important function.
Little was known about the entorhinal cortex until 2005, when the Mosers discovered grid cells and found the brain’s seat of space and navigation in the middle part of the brain structure. In 2018, they discovered in the outer end of the entorhinal cortex, a network of brain cells that sort our experiences into the right order, like beads on a string. The sequencing of experiences forms the building blocks of our sense of time.
Cell death starts decades before symptoms are noticeable
The entorhinal cortex gives rise to two brain functions that are fundamental to our ability
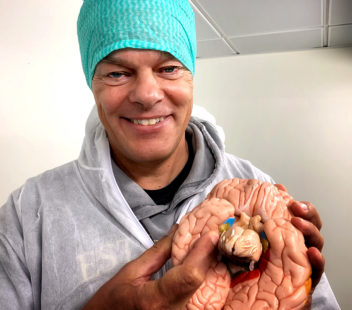
A brain that has been deeply affected by Alzheimer’s disease can shrink to the weight of an orange. “We know where in the cortex the disease first manifests itself — deep in the brain in an area the size of a fingernail that is called the entorhinal cortex,” says Edvard Moser. Photo: Rita Elmkvist Nilsen / Kavli Institute for Systems Neuroscience
to make sense of the world: the ability to translate the continuous flow of impressions and events into separate experiences with unique addresses both in space and in time.
It is also the starting point for the massive cell death that works its way through the brain, resulting in the devastating loss of cognitive function that we have come to know as Alzheimer’s disease.
We know that special neurons in the entorhinal cortex are the very first in the cerebral cortex to die from the disease. This cell death starts decades before the earliest symptoms are noticeable.
So it is not surprising that confusion about time and place, getting lost on familiar paths, or having difficulty remembering what you did yesterday or just moments ago are among the earliest symptoms of Alzheimer’s disease.
“Our sense of space and time are among the very first brain functions that are impaired in Alzheimer’s,” says Edvard Moser.
- You might also like: Kavli Institute researchers discover new type of brain cell
Must explore the early mechanisms of the disease
The Jebsen researchers believe there are several reasons why there has been so little progress in the Alzheimer’s field in recent decades.
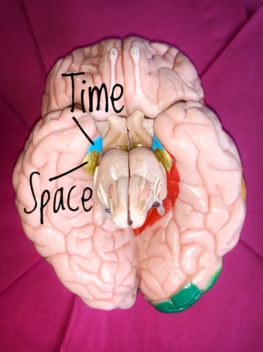
This plastic model of a human brain shows the location of our sense of space in gold, and the sense of time in sky blue. Together, these two areas make up the entorhinal cortex. The brain’s centre for memories, the hippocampus, is also found here, but it is hidden behind and tightly interwoven with the entorhinal cortex. Photo: Rita Elmkvist-Nilsen / Kavli Institute for Systems Neuroscience
One reason may be that researchers intervene too late in the course of the disease, when large parts of the brain have already been affected and damaged. Another reason is likely that researchers have conducted their experiments on types of brain cells other than the special entorhinal neurons that are naturally affected by the disease at an early stage.
It is precisely here, in the brain regions where place, time and memory occur, that researchers from the new Jebsen centre will focus their attention.
“If we are to understand what causes Alzheimer’s, we need to identify the early mechanisms of the disease in the particular area where it occurs. We need to uncover reliable biomarkers of the disease which we can use to develop an early diagnosis. Knowledge about the very first route the disease makes may enable us to intervene in the process and stop the disease before cells die and brain functions start to unravel,” says Edvard Moser.

These Alzheimer’s rats, Kristiane and Gerda, were both named after Kristian Gerhard Jebsen. Postdoc Asgeir Kobro-Flatmoen holds Gerda, and Edvard Moser has Kristiane. Alzheimer rats carry two mutations in one gene that often result in Alzheimer’s disease. Kobro-Flatmoen says when the Alzheimer rats get old, researchers notice that they have a harder time orienting themselves. Photo: Rita Elmkvist Nilsen / Kavli Institute for Systems Neuroscience
The new centre will bring together Alzheimer’s specialists across disciplines to collaborate on a set of projects designed to bridge the gaps from basic science to clinical implementation. The centre’s research will tackle everything from basic research in rats and mice to clinical research in humans. Each step, from the lab to the patient, will be quality assured with what is called translational research.
Here, promising basic research results on healthy brains will be translated to brains that have been affected by Alzheimer’s disease, and the most significant findings from human brain disease will be translated into animal models for testing before being introduced to humans.

Pictured from left: Pål Richard Romundstad, Vice Dean for Research at NTNU’s Faculty of Medicine and Health Sciences; Anne Marie Haga, director of awards, Foundation Stiftelsen Kristian Gerhard Jebsen; Sveinung Hole, managing director, Foundation Stiftelsen Kristian Gerhard Jebsen; Professor Edvard I Moser, scientific director, Kavli Institute for Systems Neuroscience, Kay Gastinger, managing director, Kavli Institute for Systems Neuroscience; Björn Gustafsson, Dean of NTNU’s Faculty of Medicine and Health Sciences. Photo: Hans W Gullestad / the Stiftelsen Kristian Gerhard Jebsen Foundation.
Officially opens 1 October
Edvard Moser and May-Britt Moser will lead the translation of Nobel Prize winning research from bench to bedside. The centre will be located at Øya Campus in Trondheim and will unite university and hospital and link them with prominent national and international partners.
The Jebsen researchers will also have access to state-of-the-art technology. This includes the 7-Tesla brain imaging machine from NORBRAIN 2, which can be used for both basic and clinical research in patients. In the fall of 2019, the MRI machine was hoisted below the ground on the hospital floor (see video).
Video: Nils Lian and Geir Otto Johansen / NTNU and St. Olav’s hospital
The national research centre was made possible by a donation from the Foundation Stiftelsen Kristian Gerhard Jebsen of NOK 22.5 million. The Central Norway Regional Health Authority has contributed NOK 11.25 million and NTNU’s Faculty of Medicine and Health Sciences has contributed NOK 5.63 million. The National Association for Public Health, with its expertise and close contact with patients and relatives, will collaborate closely with the centre.
The K. G. Jebsen Centre for Alzheimer’s Disease will officially open on 1 October 2020, and the money will fund five years of operation.





