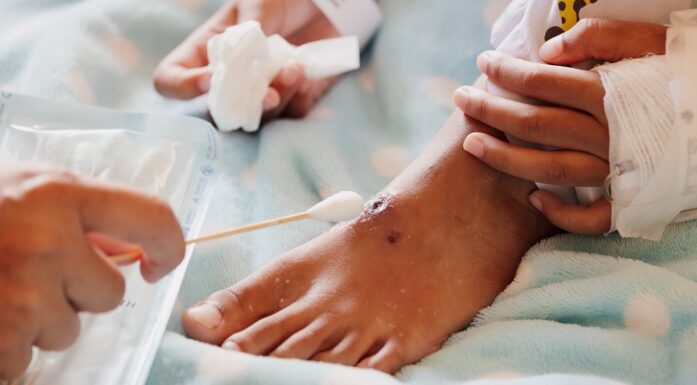
Hope for new antibiotic that was discovered by accident
Cancer researcher Marit Otterlei made a chance discovery of a brand new antibiotic that has proven effective after several experiments.
It all happened by chance.
It was a hot summer day nine years ago. Inside the laboratory, the team was working on cancer research. On the lab bench, various medications were being tested on cancer cells.
But it was getting too hot, and the work day was far from over. Someone opened the window and let in the cool summer air.
A few days later, Professor Marit Otterlei found out that there had been an infection in some of the cancer cells.
Turns out more than cool summer air was coming in through the window.
“We had a bacterial infection in some of the cancer cells. That kind of thing can happen,” Otterlei said.
- You might also like: Combination drug treatment for COVID-19 in cell culture tests
Research is far from free
That’s when they discovered it. The cancer cells that had peptides added to them had not become infected. All these particular cells were completely normal.
Simply put, a peptide is a compound consisting of a limited number of amino acids linked together. Amino acids are the building blocks of all living material.
“I thought it must mean that our peptides have an antibacterial effect,” says Otterlei. She tested the discovery a bit more and confirmed the previous result: the peptides prevented the bacteria from growing.
Right then, she was in the middle of a cancer research project. That’s really what she does. She shelved the peptide project, and continued with her work as a cancer researcher.
“Then I thought about it a little and applied for funding to test the discovery properly,” says Otterlei.
She got it.
So far, she has received over 5.6 million Euro in funding. Recently, the Trond Mohn Foundation gave almost 2 million Euro towards the research. The rest of the funding came from the Research Council of Norway, NTNU and Oslo University Hospital.
It may have been a wise investment.
- You might also like: Getting the body to make its own cancer drugs
The bacteria are still ahead
Otterlei has completed several of the steps towards an antibiotic that you and I can enjoy. Quite simply, we may enjoy it so much that we’re able to survive an infection.
It’s urgent. For decades, scientists have said it is urgent. That it’s a crisis. That someone has to cough up the money it costs to develop new antibiotics, and soon. Otherwise, people will die from something as common as a cut on the finger. Or a caesarean section. Or a bacterial pneumonia that develops, perhaps connected with a viral infection like COVID-19.
Antibiotics have long been a gift to humanity, ever since they were first discovered in a mushroom. Antibiotics can help fight tonsillitis, pneumonia, skin infections and blood poisoning caused by bacteria.
To put it even more clearly: Only one or two types of antibiotics now work against multi-resistant yellow staphylococci, which can typically cause infections in wounds or cause pneumonia, for example. This is a major problem worldwide.
And when this antibiotic stops working? It’s almost too scary to think the thought.
Because the bacteria are ahead. They know the art of mutating.
All cells have to copy their genetic material before they can divide into two cells. Bacteria have a great ability to make changes in the genetic material. They easily make new variants of themselves with slightly new features. The new variants may be more resistant to antibiotics.

For decades, scientists have said the antibiotic problem is urgent. That it’s a crisis. That someone must soon cough up the money it costs to develop new antibiotics. Otherwise, people will die from something as common as a cut on their finger. Professor Marit Otterlei now hopes that the antibiotic she discovered can be developed for commercial use. Photo: Geir Mogen / NTNU
The bacterium has become antibiotic resistant.
1-0 for the bacteria.
A kind of fertilization between bacteria
There are two ways bacteria can become resistant to antibiotics.
One way is for a common bacterium to encounter an antibiotic resistant bacterium. This can happen in hospitals or in our gut where we have lots of different types of bacteria. The bacteria form a kind of alliance. Or call it conception. The common bacterium absorbs the genetic material of the antibiotic resistant bacterium. This genetic material can contain genes that encode antibiotic resistance, and lo and behold – now the common bacterium is also antibiotic resistant.
This is how antibiotic resistance spreads.
The other way a bacterium can become resistant is for a human, fish or animal to take antibiotics for a long time. This stresses the bacterium and the bacteria will mutate inside the body or animal, developing variants that cannot be broken down by antibiotics. This ability to mutate can be compared to a super-efficient evolution, a kind of “evolution on speed”, to adapt to new environments. In this case: the presence of antibiotics.
The Otterlei peptides can kill bacteria that have become resistant either way, but of special interest is that the low-dose peptides hinder the bacteria’s super-efficient ability to mutate.
Otterlei did more thorough testing.
Peptides worked superbly
After running tests in the laboratory, the peptides were first mixed into a wound ointment and tested on a mouse infection.
Afterwards, another type of experiment was performed on rats.
There are two ways a bacterium can become resistant to antibiotics. One way is that a common antibiotic-sensitive bacterium encounters an antibiotic-resistant bacterium. The other way a bacterium can become resistant is that a human, fish or animal takes antibiotics for a long time. Illustration Photo: Colourbox
“The experiment on mice and rats showed that the peptide worked beautifully,” says Otterlei.
What the peptide does, in short, is to hinder the ability of the bacteria to copy its genetic material, causing it to die out. Obviously, Otterlei isn’t using just any old peptide.
She has created a special variant that is described academically as follows (take a deep breath and sit tight):
“In this work we show that the PCNA binding motif, APIM, from eukaryotes, also binds to the prokaryotic PCNA homologue ß-clamp. This causes cell-penetrating peptides containing APIM to prevent bacterial polymerases from performing their function. This leads to replication stops with subsequent cell death. ”
After a discovery due to an open window nine years ago, the researchers are at the point that they know the antibiotic works. Their research article has been published in a prestigious journal.
The discovery has been patented, and they still have not used most of the financial funding they have received. Now the next step is almost as difficult: turning their discovery into a drug.
Game of “snakes and ladders” to develop new medicine
“It’s almost like a Snakes and Ladders game where if you fall off the ladder you have to start all over again,” says Otterlei.
What happens is that researchers first have to decide exactly which peptides to use and in what form.
Should the final product be an ointment? Pills? Taken intravenously? Or mixed into the adhesive used to bond prostheses in the body? Once this decision has been made, specific tests need to be performed in two different animal species, using a treatment program that is the same as what you intend to use on humans.
Only then can the first human clinical trials happen.
Otterlei has not yet chosen an application field, but is still testing the peptide in various animal models. The optimal situation is to find a disease – like pneumonia – that is treated in the same way, such as intravenously, as many other infectious diseases are. Testing in this way for one purpose opens the door to obtaining broader approval for similar treatments later.
“If you choose too narrow an application initially, like a wound ointment, you have to start all over with new animal experiments to develop the peptide into something that could be given intravenously, for example,” says Otterlei.
After that, you probably need a pharmaceutical company to develop it commercially. Before humanity can get something that we really need, big industry has to make sure that they’ll make money from it.
This is often where progress grinds to a halt.
Developed new antibiotics but went bankrupt
“Last year, two companies in the US had developed and gotten approval for two new antibiotics. The medicines seemed a little better than the ones being used today. They had significantly fewer side effects and were both in a group of antibiotics with few alternatives available today. All the financial calculations had indicated that this was good business. But new antibiotics usually get saved to be a last bulwark of defence, in order to prevent the resistance to these developing as well,” says Otterlei.
And it was precisely because the drug was seen as a final defence that it got cut.
Sales were slow because doctors wanted to save lives. They wanted to keep the new drug as a back-up for when nothing else worked. Given the huge investments the companies had to make, sales were too low. Both went bankrupt.
2-0 for the bacteria.
“Although the world really needs new antibiotics, it can be bad business for companies. Developing them takes too long, and there should be a quicker path for that to happen,” says Otterlei.
In the meantime, the bacteria keep mutating.
3-0.