Why failing hearts love hard workouts
High-intensity interval training strengthens the heart even more than moderate exercise does. Now researchers have found several answers to what makes hard workouts so effective.
“Our research on rats with heart failure shows that exercise reduces the severity of the disease, improves heart function and increases work capacity. And the intensity of the training is really importance to achieve this effect,” says Tomas Stølen, a researcher at NTNU.
Stølen and his colleague Morten Høydal are the main authors of a comprehensive study published in the Journal of Molecular and Cellular Cardiology. The researchers went to great lengths to investigate what happens inside tiny heart muscle cells after regular exercise.
“We found that exercise improves important properties both in the way heart muscle cells handle calcium and in conducting electrical signals in the heart. These improvements enable the heart to beat more vigorously and can counteract life-threatening heart rhythm disorders,” says Stølen.
Fine-tuned machinery
For a heart to be able to beat powerfully, regularly and synchronously, a lot of functions have to work together. Each time the heart beats, the sinus node – the heart’s own pacemaker – sends out electrical impulses to the rest of the heart. These electrical impulses are called action potentials.
All the heart muscle cells are enclosed by a membrane. At rest, the electrical voltage on the inside of the cell membrane is negative compared to the voltage on the outside. The difference between the voltage on the outside and the inside of the cell membrane is called the resting membrane potential.
When the action potentials reach the heart muscle cells, they need to overcome the resting membrane potential of each cell to depolarize the cell wall. When this happens, calcium can flow into the cell through channels in the cell membrane.
Calcium initiates the actual contraction of the heart muscle cells. When this process is complete, calcium is transported out of the cell or back to its storage site inside each heart muscle cell. From there, the calcium is ready to contribute to a new contraction the next time an action potential comes rushing by.
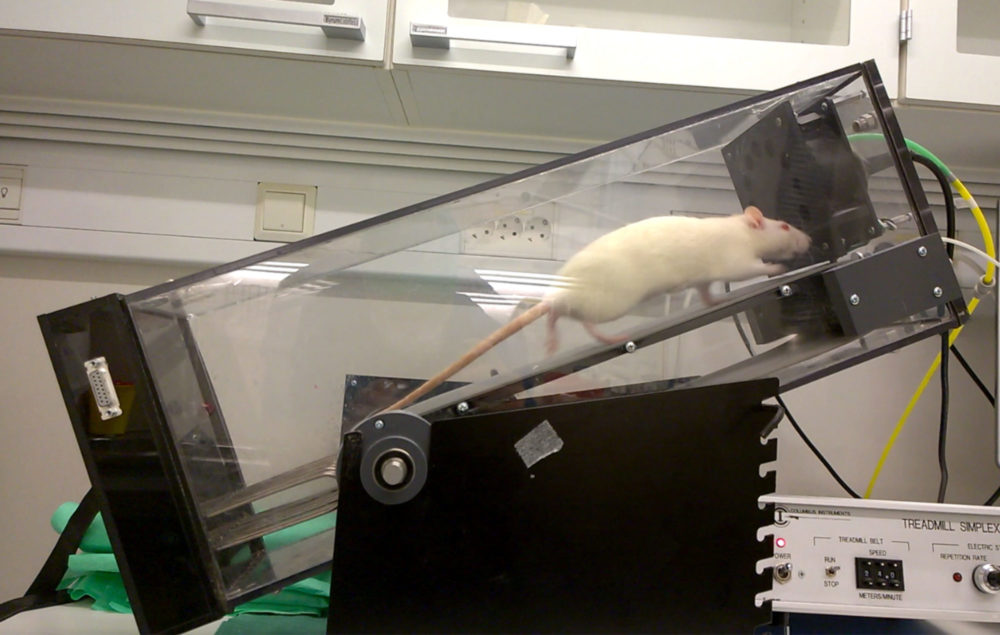
Research on rats with heart failure shows that exercise reduces the severity of the disease, improves heart function and increases work capacity. Photo: NTNU
If the heart’s electrical conduction or calcium management system fails, the risk is that fewer heart muscle cells will contract, the contraction in each cell will be weak, and the electrical signals will become chaotic so that the heart chambers begin to flutter.
“All these processes are dysfunctional when someone has heart failure. The action potentials last too long, the resting potential of the cells is too high, and the transport function of the calcium channels in the cell wall is disturbed. Calcium then constantly leaks from its storage places inside every heart muscle cell,” Stølen says.
Before Stølen gives us the rest of the good news, he notes, “Our results show that intensive training can completely or partially reverse all these dysfunctions.”
- You might also like: Keeping the spark lit into the golden years
100,000 weak hearts
Normally, the sinus node causes a human heart to beat between 50 and 80 beats every minute when at rest. This is enough to supply all the organ systems and cells in the body with as much oxygen-rich blood as they need to function properly.
When we get up to take a walk, our heart automatically starts beating a little faster and pumping a little harder so that the blood supply is adapted to the increased level of activity. The higher the intensity of the activity, the harder the heart has to work.
Exercise strengthens the heart so it can pump more blood out to the rest of the body with each beat. Thus, the sinus node can take it a little easier, and well-trained people have a lower resting heart rate than people who have not done regular endurance training.
At the other end of the continuum are people with heart failure. Here the pumping capacity of the heart is so weak that the organs no longer receive enough blood to maintain good functioning. People with heart failure have a low tolerance for exercise and often get out of breath with minimal effort.
In other words, increasing the pumping power to the heart is absolutely crucial for the quality of life and health of people with heart failure.
- You might also like: Hope for new antibiotic that was discovered by accident
High intensity intervals
Many of the more than 100 000 Norwegians who live with heart failure have developed the condition after suffering a major heart attack – just like the rats in Stølen and Høydal’s study.
In the healthy rats, the heart pumped 75 per cent of the blood with each contraction. In rats with heart failure, this measure of pump capacity, called ejection fraction, was reduced to 20 per cent, Stølen says.
The ejection fraction increased to 35 percent after six to eight weeks with almost daily interval training sessions on a treadmill. The rats did four-minute intervals at about 90 per cent of their maximum capacity, quite similar to the 4 × 4 method that has been advocated by several research groups at NTNU for many years.
“The interval training also significantly improved the rats’ conditioning. After the training period, their fitness level was actually better than that of the untrained rats that hadn’t had a heart attack,” says Stølen.
- You might also like: Getting the body to make its own cancer drugs
Prevents life-threatening arrhythmia
Impaired calcium handling in a heart muscle cell not only causes the cell to contract with reduced force every time there is an action potential. It also causes the calcium to accumulate inside the fluid-filled area of the cell – the cytosol – where each contraction begins.
The calcium stores inside the cells are only supposed to release calcium when the heart is preparing to beat. Heart failure, however, causes a constant leakage of calcium out of these stores. After each contraction, calcium needs to be efficiently transported back into the calcium stores – or out of the heart muscle cell – via specialized pumps. In heart failure patients, these pumps work poorly.
When a lot of calcium builds up inside the cytosol, the heart muscle cells can initiate new contractions when they’re actually supposed to be at rest. An electrical gradient develops which causes the heart to send electrical signals when it shouldn’t. This can cause fibrillation in the heart chambers. This ventricular fibrillation is fatal and a common cause of cardiac arrest.
“We found that interval training improves a number of mechanisms that allow calcium to be pumped out of the cells and stored more efficiently inside the cells. The leakage from the calcium stores inside the cells also stopped in the interval-trained rats,” says Stølen.
The effect was clear when the researchers tried to induce ventricular fibrillation in the diseased rat hearts: they only succeeded at this in one of nine animals that had completed interval training. By comparison, they had no problems inducing fibrillation in all the rats with heart failure who had not exercised.
- You might also like: People with atrial fibrillation live longer with exercise
Micromolecules to the rescue
So far, the research group had shown that exercise improves calcium management in diseased heart muscle cells in several ways. The training also makes the electrical wiring system of the heart more functional.
In addition, they showed that exercise counteracted processes that cause the heart to become big and stiff.
Taken together, these improvements make each heartbeat more powerful and reduce the severity of heart failure. The risk of dangerous ventricular fibrillation was also reduced.
But Stølen and team still lacked an answer to why exercise corrects slow action potentials and ensures that the heart muscle cells are able to take care of calcium in the right way.
Therefore, they investigated whether the training had altered the genetic activity inside the rat cells. Thousands of different types of micromolecules called micro-RNA probably control most of this activity through direct interaction with genes.
“It turned out that 55 of the micro-RNA variants we examined were altered in rats with heart failure compared to the healthy rats. Interval training changed 18 of these back towards healthy levels. Several of the relevant micromolecules are known to play a role in both calcium management and the electrical conduction system of the heart, but the most interesting thing is that we discovered new micro-RNAs that can play an important role in heart failure,” says Stølen.
- You might also like: Hope for 500 000 insomniacs in Norway
Moderate training also of some benefit
This article has mostly considered the effects of high-intensity interval training. But the study also includes a group of rats that trained more sedately.
The rats in this group ran the same distance and thus did as much total training work as the rats in the interval training group. However, they had to exercise longer each time since they trained at a lower intensity. Stølen notes that this form of training also resulted in several health improvements.
But, he emphasizes, the vast majority of improvements were greater with interval training. “For example, we were able to induce cardiac fibrillation in five of eight rats after a period of moderate exercise, and their pumping capacity had only improved half as much as in the interval training group.”
Reference: Tomas O. Stølen, Morten A. Høydal et al: Exercise training reveals micro-RNAs associated with improved cardiac function and electrophysiology in rats with heart failure after myocardial infarction. Journal of Molecular and Cellular Cardiology.
https://doi.org/10.1016/j.yjmcc.2020.08.015






