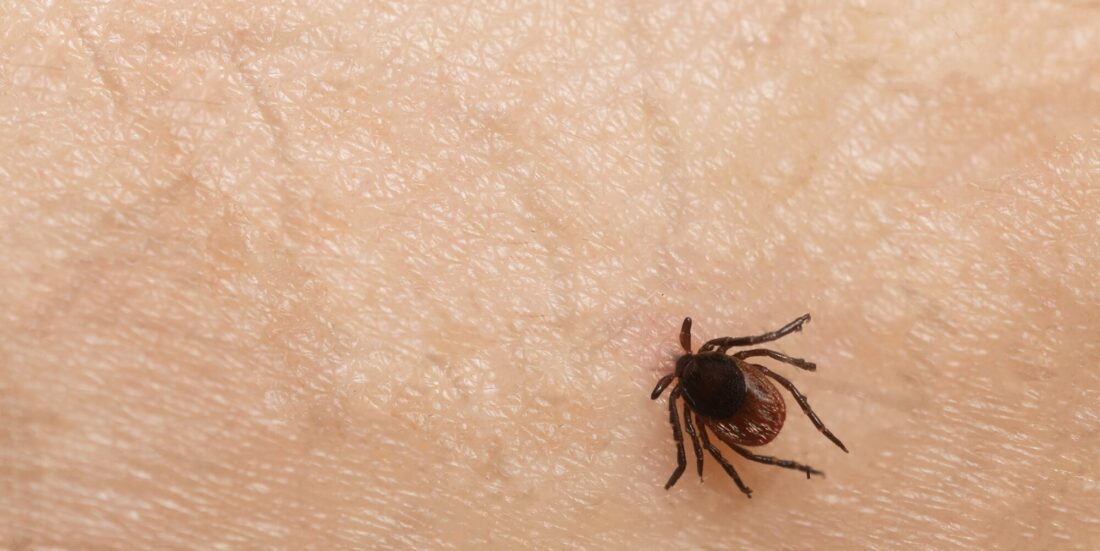
Study finds no evidence of persistent tick-borne infection in people who link chronic illness to ticks
When researchers studied Norwegians who blamed tick bites for their chronic health problems, they found no objective evidence that ticks were the cause.
In brief
- A study of 470 Norwegians who attributed long‑term health problems to tick bites found no objective evidence linking their persistent symptoms to ongoing tick‑borne infections.
- Participants reported significant issues—including fatigue, low physical activity, and reduced ability to work—but blood tests did not show active infection as the cause.
- While 37.5% had antibodies indicating past exposure to Lyme‑related bacteria, the study found no association between these antibodies and chronic symptoms.
- Researchers emphasize the importance of accurate diagnosis and caution against unnecessary long‑term antibiotic treatments, noting that misdiagnosis can overlook other health conditions.
This summary was written by AI and was checked for accuracy by a human journalist.
Many Norwegians pull ticks from their bodies every single summer. Roughly 2 per cent of those who are bitten are infected by a bacterium that leads to Lyme disease.
The disease can start with a rash that eventually spreads on the skin in a ring-shaped pattern. In some people, the disease can develop into facial paralysis, meningitis or other complications.
Can develop facial paralysis
“It’s possible to get really sick from tick bites, but no matter how badly you are affected, antibiotics are the curative treatment. Most people need two weeks of treatment, while a few need up to four weeks,” says Audun Olav Dahlberg.

“I myself am very fond of outdoor activities, and wanted to find out more about the different connections between ticks and disease,” says Audun Olav Dahlberg, senior consultant at Møre og Romsdal HF Health and doctoral fellow at NTNU. Photo: Private
Dahlberg is a senior consultant in clinical neurophysiology at Helse Møre og Romsdal HF, and is a specialist in clinical neurophysiology and neurology as well as a PhD research fellow at NTNU.
As part of his doctoral dissertation, he examined 470 Norwegians who themselves link chronic and long-term health problems to tick bites.
His research found no evidence that the chronic health problems reported by this group are linked to ongoing tick-borne infections.
The study also shows that around 0.12 per cent of adults in Norway link chronic health problems to previous tick bites.
Depression, sick leave and exhaustion
“This is the first time that we have quantified how many people in Norway themselves link chronic health problems to tick bites. This group suffers greatly, including from a limited ability to work, severe fatigue and other health issues. Their symptoms have persisted for more than six months and they believe tick bites are the cause. However, blood tests indicate that active tick-borne infection cannot explain these persistent symptoms,” says Dahlberg.
To recruit participants, the researchers sent SMS messages to 270,000 people randomly drawn throughout Norway, while GP offices, the Norwegian National Advisory Unit on Tick-borne Disease and the Norwegian Lyme Borreliosis Disease Association also helped with the recruitment.
A total of 470 participants were examined and compared with control groups. All were over 18 years old, and had had symptoms for more than six months.
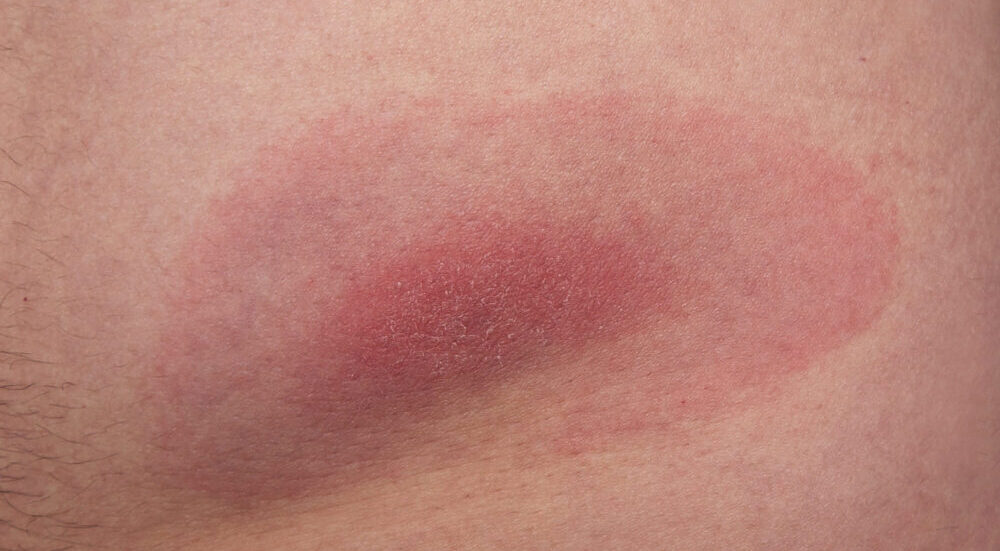
Lyme disease can start with a rash that spreads across the skin in a ring-shaped pattern. PhD research fellow and medical doctor Dahlberg emphasizes that people should contact a doctor if symptoms develop after a tick bite, so that the correct treatment can be assessed and possibly initiated. Ill photo: Colourbox
More than one in three have Lyme disease antibodies
Persistent symptoms were most prevalent in areas with a lot of ticks. In South-Western Norway, around 0.15 per cent had problems attributed to tick bites, while the percentage in Northern Norway was just 0.03 per cent.
Among the participants, 37.5 per cent had antibodies against the bacterium that most often causes Lyme disease. This shows that many people have been in contact with the bacterium and developed an immune response.
The participants also had antibodies against Borrelia and other tick-borne microbes more often than the control group. However, the study found no proven association between these antibodies and the persistent symptoms.
The study shows that 23 per cent of the participants had been diagnosed abroad. Dahlberg says this raises questions regarding the diagnostic methods used in some countries, as some laboratories use test methods that are not in line with established professional practice.
How the study was conducted
- The researches reviewed medical records from the patient's GP or medical specialist.
- Blood samples from each participant were analyzed
- The participants were examined using recognized questionnaires for physical symptoms, assessment of fatigue, physical health and mental symptoms
- Antibiotic treatment and treatment plan for each participant was assessed
- Blood samples were checked for antibodies against Borrelia burgdorferi sensu lato, encephalitis virus (TBEV), Francisella tularensis, Coxiella burnetii, Anaplasma phagocytophilum, Babesia spp., Bartonella spp., and Rickettsia spp.
- Blood samples were also examined for active infections by B. burgdorferi, B. miyamotoi, phagocytophilum, Rickettsia spp., Neoehrlichia mikurensis, F. tularensis, Bartonella spp., and C. burnetii
Important to get correct diagnosis
“We have thoroughly investigated whether ticks can explain the suffering in this group of participants. Since the study found no link between persistent symptoms and ongoing infection, it can contribute to more targeted follow-up and treatment. Objective findings are important for making diagnoses, and long-term antibiotic treatment beyond established practice is not recommended. An incorrect diagnosis can lead to other medical conditions being overlooked. That makes it crucial to have a thorough investigation based on objective findings,” says Dahlberg.
Lyme disease can make you very ill. Dahlberg says this means people should see their doctor if they develop symptoms after a tick bite so that correct treatment can be assessed and possibly started.
Dahlberg emphasizes that the study’s findings apply at the group level.
“Of course, some individuals may experience long-term ailments after tick-borne infections, such as persistent nerve damage, immune responses, or a combination of biopsychosocial factors, such as psychological stress or social circumstances. However, the study shows no indications at the group level that a large number of Norwegians experience long-term symptoms that can be attributed to persistent tick infections,” Dahlberg said.
Reference: Dahlberg, A.O., Aase, A., Reiso, H. et al. Prevalence and clinical characteristics of Norwegians who report persistent health complaints attributed to tick bites or tick-borne diseases. BMC Infect Dis 25, 1663 (2025). https://doi.org/10.1186/s12879-025-12182-w