Foetal genes can increase the risk of illness during pregnancy
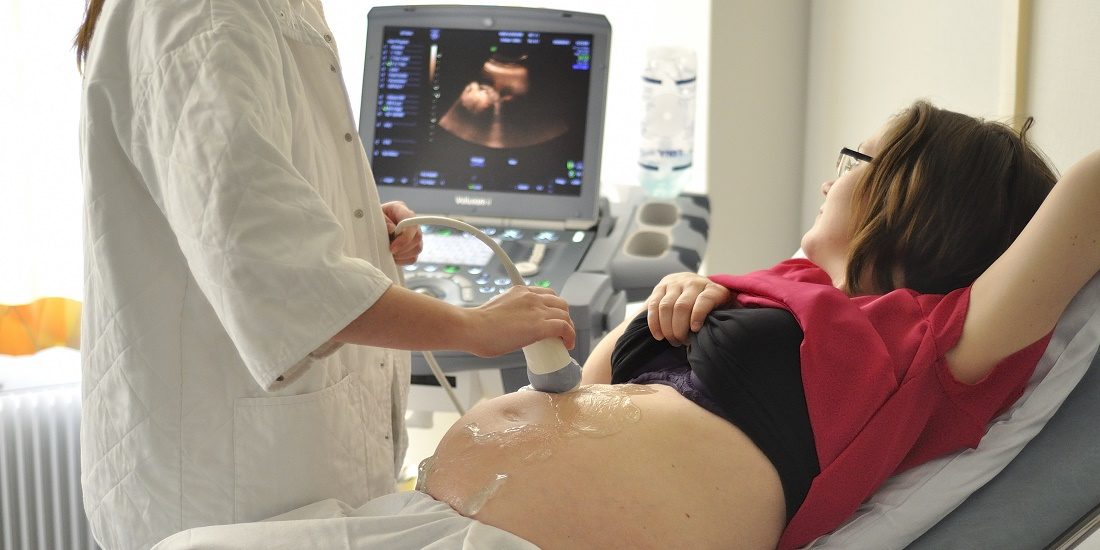
A mother’s risk of getting preeclampsia, a potentially life-threatening illness associated with pregnancy, can be linked in some cases to genes from her foetus.
For the first time, a relationship has been found between foetal genes and the risk of preeclampsia in the mother.
Norwegian researchers, including a team from NTNU, figure prominently in the international group that presented the find in Nature Genetics.
Preeclampsia affects around 3 per cent of births in Norway; worldwide, that number is estimated to be about 5 per cent.
In the vast majority of cases, the mother has mild symptoms, typically high blood pressure. Nevertheless, preeclampsia is one of the leading causes of death in both mothers and babies around the time of birth, and sometimes the only way to treat it is to deliver the baby, even prematurely.
- You might also like: Information from 30,000 pregnant women can save lives
Little studied
“For the first time ever, we have discovered a foetal gene that increases the risk of preeclampsia,” says Ann-Charlotte Iversen at the Department of Cancer Research and Molecular Medicine at NTNU.
She says there has not been much research on the role of foetal genes in triggering the illness.
Preeclampsia usually begins with a problem in the placenta, which is mainly composed of foetal cells.
For that reason, it makes sense that foetal cells might have a hand in causing the illness, Iversen said, even though it is the mother’s symptoms during the last part of the pregnancy that lead to the diagnosis.
Iversen is head of a research group at NTNU’s Centre of Molecular Inflammation Research (CEMIR).
The largest of its kind in the world
“Our findings are particularly solid for three reasons: we analysed a large number of individuals, we found several genetic variables that all point to the same gene associated with the risk, and two independent population studies confirmed that this gene is associated with the risk,” Iversen said.
There are also a number of major studies that support the conclusions. CEMIR is one of 12 partners from 6 different countries in an EU project called InterPregGen, which was created in 2011.
“We are all working together to uncover the genetic risk factors for preeclampsia in the mother and foetus. We have linked a number of major European population studies to conduct the world’s largest genetic study of preeclampsia,” says Iversen. “Our contribution to the project has been information on a group of women from the HUNT study who have had problematic and healthy pregnancies, as well as information from the Preeclampsia Biobank, which has been collected independently.”
The Nature Genetics article includes analyses of material from the Preeclampsia Biobank, including blood samples and tissue samples from placentas that have been collected at St. Olavs and Haukeland University Hospitals
- You might also like: Learning more about preeclampsia
Protein as biomarker
The genetic variants identified by the researchers are associated with the FLT-1 gene, which encodes a protein that in soluble form is known as a biomarker for preeclampsia.
The protein contributes to damaging the mother’s vascular system so that she develops symptoms such as high blood pressure and an increased amount of protein in the urine. This happens as a result of problems with the placenta, essentially because foetal cells in the placenta produce the protein.
“We have shown here that the risk of disease may be because changes in the gene affect how the protein works and how it affects the mother. This is a foetal gene that gives the mother an increased risk of developing preeclampsia. This find clearly brings us closer to a better understanding of preeclampsia,” Iversen said.

The goal of the project is to determine which mothers and children are at highest risk of preeclampsia. Photo: Colorbox
Building on established expertise
CEMIR’s contribution to the effort came in the form of three researchers: Gabriela Silva, a PhD candidate; gynaecologist and postdoctoral physician Liv Cecilie Vestrheim Thomsen (who also works at Helse Vest, the Western Norway Regional Health Authority) and Iversen herself. The research centre has solid expertise in molecular analyses of the activation of the placenta.
“The EU project has brought together geneticists, statisticians and clinicians. NTNU and CEMIR’s expertise has been a complementary strength,” says Iversen.
Gabriela Silva analysed the protein expression of FLT-1 in placental samples from sick and healthy pregnant women, while Liv Cecilie Vestrheim Thomsen has been central in collecting the placentas.
“We have compared the result with the occurrence of the genes associated with the risk. This means that we have conducted a functional follow-up of the gene discovery, which has now been published,” Iversen says.
CEMIR is one of the foremost research centres in Norway and has been selected as a Centre of Excellence by the Research Council of Norway.
- You might also like: Exercise prevents gestational diabetes in overweight women
Predicting which women will get sick
“CEMIR’s Research Group for inflammation in pregnancy has as its goal to figure out which disease mechanisms cause problems with the placenta and lead to the development of preeclampsia,” says Iversen.
The group is working to understand what goes wrong so they can detect problems early in a pregnancy. The goal is to predict which women will develop the disease.
“Our molecular analyses have identified specialized foetal cells in the placenta as the main actors in preeclampsia. These are the same foetal cells that have been identified with this new genetic discovery. This reinforces our conviction that foetal cells play an active role, and represents a big change in thinking, since research has previously focused most on the mother’s immune system. If we want to prevent preeclampsia, we have to understand the foundation for the disease,” says Iversen.
The Norwegian Mother and Child Cohort Study (MoBa), coordinated by the Norwegian Institute of Public Health, also participated in the Nature Genetics study.
In countries with more limited resources than Norway, preeclampsia can be an even bigger problem. In conjunction with their research project, the partners in InterPregGen have helped built up pregnancy-based biobanks in Central Asia, where they have been in short supply.
Reference:
Variants in the fetal genome near FLT1 are associated with risk of preeclampsia. R. McGinnis, V. Steinthorsdottir, N. O. Williams, G. Thorleifsson, S. Shooter, S. Hjartardottir, S. Bumpstead, L. Stefansdottir, L. Hildyard, J. K. Sigurdsson, J. P. Kemp, G. B. Silva, L. C. V. Thomsen, T. Jääskeläinen, E. Kajantie, S. Chappell, N. Kalsheker, A. Moffett, S. Hiby, Wai Kwong Lee, S. Padmanabhan, N. A. B. Simpson, V. A. Dolby, E. Staines-Urias, S. M. Engel, A. Haugan, L. Trogstad, G. Svyatova, N. Zakhidova, D. Najmutdinova, The FINNPEC Consortium, The GOPEC Consortium, A. F. Dominiczak, H. K. Gjessing, J. P. Casas, F. Dudbridge, J. J. Walker, F. Broughton Pipkin, U. Thorsteinsdottir, R. T. Geirsson, D. A. Lawlor, A.-C. Iversen, P. Magnus, H. Laivuori, K. Stefansson, L. Morgan. https://www.nature.com/ng/journal/vaop/ncurrent/full/ng.3895.html