Sound waves for your health
You may not be able to hear them, but they help to diagnose and treat patients every day. In the past 40 years, ultrasound imaging has gone from blurry black-and-white images, to sharp 3D images in real time. And the technology is still developing. Now, artificial intelligence is being tested for aid in interpreting ultrasound images.
Researcher and professor Lasse Løvstakken starts a video on his computer screen. We’re in the eye of a storm. It looks almost like a hurricane approaching a coastline. Is this New Orleans? No. Although the arrows circulating on the screen look a lot like a weather model, they actually represent the speed at which blood is moving through a human heart.

Lasse Løvstakken is head of the ultrasound group at the Department of Circulation and Medical Imaging. Photo: Karl Jørgen Marthinsen
This is the latest visualization of the way blood circulates around the heart. Imaging systems like this one will provide accurate measurements of detailed circulation patterns, which can help diagnose heart disease.
“We’ve been working on this since 2014, and now we’re testing it on patients,” Løvstakken explains. He’s the leader of the ultrasound group at the Department of Circulation and Medical Imaging at NTNU.
The next step will be to do the same thing for a 3D model of the heart.
From days to minutes
This way of “looking” into the heart exists thanks to a unique collaboration between doctors and engineers in Trondheim.
Forty years ago, ultrasound looked completely different. Back then, it was barely used for diagnostics. If a patient appeared to have heart issues, it would take days or weeks to get it checked. You had to go to a special lab, and go through long, risky procedures involving X-rays and catheters through your veins.
It took one to two days to process images, and it looked like porridge.
Today, you can check for the same issue within 30 minutes, without any of the invasive procedures or associated risks.
In addition to medical diagnostics, ultrasound can be used for many other important purposes, such as checking welds in steel tubing, and materials testing in the oil and gas industry.
What is ultrasound?
Ultrasound waves are sound waves at a frequency higher than the human ear is able to hear.
Ultrasound used in medical diagnostics is generally between 1-15MHz, transmitted towards a target and received by a transducer. The signal is then converted to images, signal curves or audible sound.
In general, medical ultrasound use can be divided into three categories:
- Diagnostic imaging
- Therapeutic uses at medium power, for uses such as warming up and stimulating muscles
- Therapeutic at high power, for uses such as breaking up kidney stones or treating brain conditions like essential tremors
Ultrasound was first used in diagnostics to look at the heart, known as echocardiography. Ultrasound can also be used to look at any tissue, organs, joints or large veins in the body, as well as for studying the brain, and for monitoring foetuses during pregnancy.
Ultrasound imaging uses the doppler effect to measure things like the flow rate of blood cells in an artery. Similarly to an ambulance driving past your house, the frequency of the reflected wave will vary depending on the speed of the reflector. So the frequency will be higher it a blood cell is moving towards you, and lower if it’s moving away.
Will ultrasound ever reach a limit?
Ultrasound has lots of advantages, making it a useful and exciting technology. It gives the ability to “see” into different materials without cutting into them.
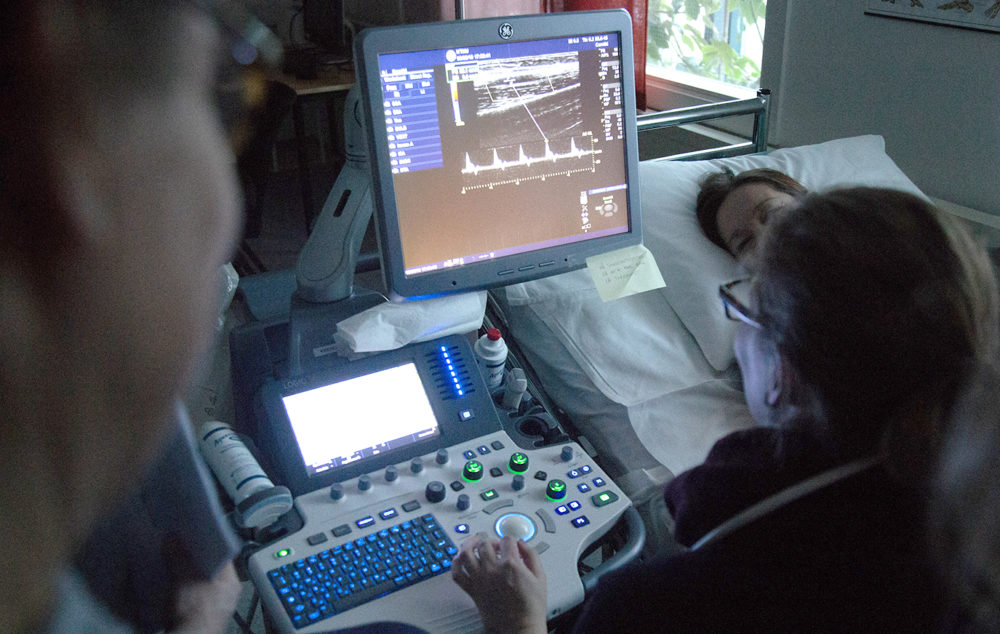
Ultrasound is constantly being developed to help diagnose, monitor and measure different processes in the body. Photo: Karl Jørgen Marthinsen
Sound waves are sent into the body and reflect back to form images the heart, liver, veins, and more. You can measure the movement of the heart and blood circulation speeds around it. These are things that can’t be measured as accurately with other methods such as CT or MRI scans. Ultrasound is a completely safe method of looking at what’s happening inside the body.
Researchers are constantly developing new ways of using ultrasound to uncover, diagnose and monitor processes in the body.
That’s part of the secret behind our development. We cover a lot of different disciplines, between physics, mathematics, image and signal processing, and digital visualization. And we work closely with doctors.
“For years now, I’ve thought, now we’ve reached the limits of what’s possible with ultrasound,” says NTNU medical technology professor Hans Torp.
He is one of the first researchers in Norway to work on ultrasound imaging in medicine. For 40 years, he has been developing solutions for the medical community centred around sound waves. He has worked closely with clinicians, who push him to find new ways to check this, or measure that.
“A lot of our ideas come from talking to doctors. They’re always in need of new tools, and asking us if it is possible to find some easier way to diagnose, interpret and monitor patients with ultrasound. And that tends to get the gears grinding.”
And there hasn’t been many times that Torp has had to give up on an idea, only if the necessary technology hadn’t been developed yet.
Interdisciplinary work
Around 200 people work at the Department of Circulation and Medical Imaging, with 60-70 of them within the ultrasound group. They are world leaders within their field of research.
“We’re in a unique position in Norway– really, in the world, with us technologists in offices at the hospital with doctors all around us. The walls are full of history about interdisciplinary work between doctors, clinicians and the industry, and it’s really special.” This is what Lasse Løvstakken thinks.
Today’s 3D images provide a real-time idea of the situation ‘beforehand’, rather than having to go into an invasive procedure with the patient as a potential Pandora’s box, Aakhus explains.
“That’s the secret behind our advances. We cover a lot of bases, between physics, mathematics, image and signal processing and digital visualization. And we work closely with doctors. It’s really exiting, and we get results quickly.”
Video game technology
Ultrasound 40 years ago was able to produce sound signals that had to be expertly interpreted to diagnose the condition of the patients’ heart. In the early 70s, doctors were able to get blurry images of slices of the heart in black-and-white. In the 80s, color doppler imaging was introduced, showing which way blood was showing in different parts of the heart. This provided even more insight, with the technology now being able to reveal shrinkage or leakages in different parts of the heart.
And the technology just keeps improving. The industry is almost as much of a driving force for solutions as the researchers are.

In addition to medical diagnostics, ultrasound can be used for many other things, such as examining welded seams in steel piping, as well as testing of different materials used in the oil and gas industry. Illustrative photo: NTB Scanpix
“We’re always hoping for better image quality. In the beginning, we just didn’t have enough computing power, and the technology wasn’t particularly advanced. There were a lot of challenges. We knew what we wanted, but just didn’t have the tools to get there yet,” Hans Torp explains. “In the past few years, we’ve had a lot of aid from the video game industry. They’ve pushed improvements in terms of computing power, fast networking, and phenomenal graphics, which has been incredibly useful for us. We couldn’t even imagine these things 30 years ago.”
Ultrasound to detect blood poisoning
Sepsis, commonly known as blood poisoning, is one of the most deadly conditions in the world. About half of deaths in Norwegian hospitals are related to sepsis. Right when sepsis begins to take effect, changes to the blood circulation in the small vessels (microcirculation) occur. Early diagnosis and treatment with antibiotics is incredibly important to help reduce fatalities, and ultrasound can often be the difference between detection early enough or too late.
Hans Torp and the sepsis group at St. Olav’s hospital/NTNU have developed a probe that uses ultrasound to help detect early changes to microcirculation and make important diagnoses.
New technology and machines give researchers access to data in new and more flexible ways. This can bring around old ideas to be tested in new ways, or allow data to be played with in new and inventive ways that bring around advances to the technology. Almost always in collaboration with the doctors.
Doppler sounds
Cardiologist and professor Svend Aakhus can attest to this.
“This is an incredibly useful tool for us,” say Aakhus, who still remembers his first experience with ultrasound as a recently graduated doctor. It was at “hjerteposten” in 1987 at Trondheim Regional Hospital, now known as St. Olavs Hospital.
“I was walking through the hallway towards the ward where the examinations were done. I heard a sound I’d never heard before coming out of the door of the dark room. Swoosh, swoosh, swoosh– as it turns out, it was the characteristic doppler sound. When I started to understand what ultrasound could be used for, I thought it was just fantastic.”
From Pandora’s box to having foresight
The latest technology is a 3D image of the heart’s valves taken through the esophagus. This is done before heart surgery, and is on a screen during the operation as well.
“With the 3D images we have today, you get a real time representation of the situation beforehand, rather than having to go into an invasive procedure blind, with a patient that’s a potential pandora’s box,” Aakhus explains.
The first 3D images were introduced in the early 90s, with Duke University in the USA presenting the first 3D echocardiography machine. It was the size of four refrigerators and a probe the size of a kilo block of butter.
“It took several days to process the images, and the result looked like porridge,” he said.
The video shows a 3D visualization of blood flowing through the heart. An accurate method of measurement like this can provide vital information for diagnosing different heart conditions. Video: Department of Circulation and Medical Imaging, NTNU
Sven Aakhus reminisces, smiling.
“25 years later, ultrasound images are practically like looking at reality itself. It’s been a huge determining factor in our success. It allows us to take a completely different approach, which is fantastic. We knew what we wanted, we just had to wait for the technology and computing power to catch up.”
Extension of the arm
The drastic increase in image quality has made ultrasound diagnostics indispensable for clinical use. So the doctors need to keep up.
NeoDoppler
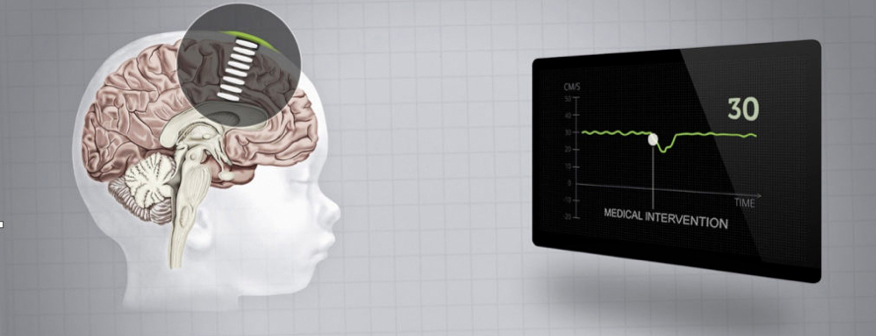 NeoDoppler is a little ultrasound device that can help prevent brain injuries in premature babies. The risk of brain injury is very high in the first few days after a premature birth, so it’s very important to monitor the blood flow to the brain for any potential instabilities.
NeoDoppler is a little ultrasound device that can help prevent brain injuries in premature babies. The risk of brain injury is very high in the first few days after a premature birth, so it’s very important to monitor the blood flow to the brain for any potential instabilities.
The sensor and probe that Hans Torp has developed is attached to a premature baby’s fontanelle, and ultrasound measures blood flow throughout the brain simultaneously, which has been a challenge to develop.
The same technology can also be used to find calcifications of veins in the legs. This is very difficult to detect at an early stage, and the condition can sometimes lead to amputation.
Today, ultrasound probes are practically an extension of clinicians’ arms. One of the advantages of ultrasound technology is that the devices can be made small and portable, so that doctors can bring the devices to the patients. This miniaturization means that ultrasound imagers are available everywhere and can be used outside of hospitals.
“We wouldn’t be able to do modern cardiology without ultrasound,” Aakhus points out.
And more and more groups are introducing ultrasound to their toolboxes.
“Experiments to interpret ultrasound images with artificial intelligence have started.”
It’s not just cardiology that uses ultrasound. X-ray doctors have used it for years. As have gynecologists and midwifes. Neurology uses ultrasound to image veins and arteries in the neck and brain, and rheumatologists have started using it to look at muscles and joints. Digestion specialists have also been looking into ultrasound uses in their field.
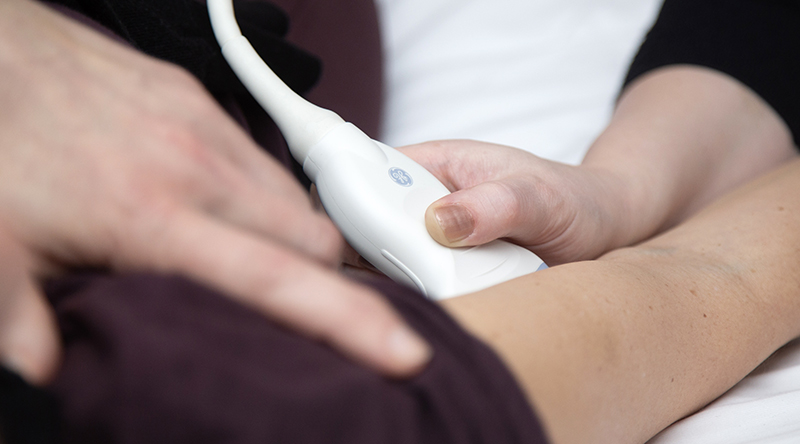
Ultrasound can be found in practically every department at the hospital. Photo: Karl Jørgen Marthinsen
Ultrasound is an important guide for taking biopsies and draining fluids in the pericardium, pleural sac and stomach cavity. With an ultrasound imager, the doctor is able to see their needle and make sure that it goes into the right place. It’s a good tool to have.
Artificial intelligence and ultrasound
Experiments to use artificial intelligence for interpreting ultrasound images are now underway at NTNU.
“We want computer technology that can interpret easily recognizable features in ultrasound images. Machine learning can help make a doctor more effective and precise in their work, and maybe be able to point out if something is wrong,” says Lasse Løvstakken. His department now has a project working on developing a program that can recognize fibrosis in the heart. This isn’t particularly easy to see, and it’s hard to see how much there is. Hopefully, AI will be able to make things easier.
“What’s the next big thing in ultrasound?”
Løvstakken thinks for a second.
“There’s a lot happening on the technology side of things right now. We’re constantly getting upgraded ultrasound probes with even more technology in them. Miniaturization will continue, and, even though doctors still need to learn the analysis, more things will be able to be detected automatically. 3D imaging at full resolution is right around the corner, and totally new technologies for sending and receiving sound are in the works. All of this will help make patient treatments better– and build a base for new solutions. It’s never going to end!”







